On April 22, 2014, the NEJM Knowledge+ Question of the Week focused on the most appropriate next step in care for a patient with hereditary hemochromatosis who was being treated with therapeutic phlebotomy but whose laboratory results showed signs of mild anemia.
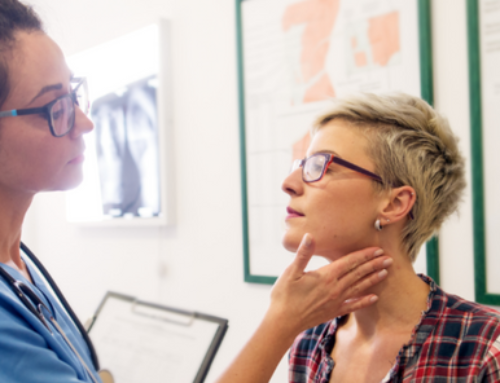
More than 1800 physicians answered the question, and an interesting pattern emerged in their responses. As shown below, about one-third of respondents chose to continue therapeutic phlebotomy (the correct answer), but an equal proportion chose to discontinue phlebotomy and begin iron chelation therapy.
a. Discontinue phlebotomy and restrict dietary iron intake (18%)
b. Perform CT of the liver (11%)
c. Discontinue phlebotomy and begin iron chelation therapy (32%)
d. Discontinue phlebotomy and initiate vitamin C supplementation (7%)
e. Continue therapeutic phlebotomy (32%)
To better understand these results and what we might learn from them, we talked to Dr. Jason Gotlib, Associate Professor of Medicine (Hematology) at Stanford University School of Medicine.
Q: What is your initial reaction to these results?
A: I’m not necessarily surprised that a moderate proportion of respondents chose answer C, which is to discontinue phlebotomy and begin iron chelation therapy. Different physicians may have different levels of comfort about the level of anemia that would persuade them to discontinue phlebotomy and transition to iron chelation therapy.
Q: What is the clinical rationale for continuing therapeutic phlebotomy in the setting of anemia? Is there any particular level of anemia at which you would indeed stop the phlebotomy and start iron chelation?
A: Various methods for approaching phlebotomy endpoints have been undertaken. A common practice used in hematology, which is reflected in answer E, is to phlebotomize patients with hereditary hemochromatosis on a weekly basis until iron-deficient hematopoiesis develops. Iron-deficient hematopoiesis manifests as a decrease in hemoglobin concentration and mean corpuscular volume (to the low 80s), a decrease in transferrin saturation to 10%–20%, an increase in total iron-binding capacity (TIBC; transferrin) to >300 μg/dL, and a reduction in the serum ferritin concentration to the low-to-normal range (5–10 ng/mL).
I would not be deterred from continuing phlebotomy in a patient who develops mild anemia (as in this case, with a hemoglobin level of 11.7 g/dL), particularly if the ferritin and transferrin saturation levels remain higher than the desired endpoints for iron-deficient hematopoiesis (as was the case here). A reasonable way to achieve these endpoints is to continue phlebotomy until the hemoglobin concentration (g/dL) drops into the low 11s or the high 10s. In such cases, iron deficiency does not require treatment because increased gut absorption of iron from food will improve or reverse the anemia within several weeks after phlebotomy is stopped.
An alternative approach is to have patients undergo weekly phlebotomy until normal iron stores are realized. For example, goal iron indices include a ferritin level of <50 ng/mL and transferrin saturation of <50%. In this approach, iron-deficient hematopoiesis is not pursued as a phlebotomy goal, and phlebotomy is halted if the hemoglobin level or hematocrit decreases by more than 20% from baseline (Hepatology 2011; 54:328). In this case, the patient’s baseline hemoglobin level is not provided, so the extent and pace of hemoglobin change over time is unclear. However, we know that the patient’s hemoglobin concentration is 11.7 g/dL, and this relatively mild anemia would not be enough to dissuade me from continuing phlebotomy at this point in time.
Maintenance phlebotomy should be continued in hereditary hemochromatosis patients after primary iron depletion to prevent reaccumulation of iron. A goal serum ferritin concentration between 50 and 100 ng/mL is commonly pursued, and this can be achieved in most patients by having them undergo a 500-mL phlebotomy every 2 to 4 months.
Q: Are there any clinical situations where even mild anemia might trigger you to switch from phlebotomy to iron chelation therapy?
A: Intolerance of phlebotomy (e.g. congestive heart failure with unstable hemodynamics) can be an indication for iron chelation therapy. Phlebotomy is usually effective enough to achieve iron-deficient hematopoiesis and/or normal iron stores, and a switch to iron chelation therapy is not usually required. However, in patients with comorbid medical conditions associated with pre-existing anemia (e.g., myelodysplastic syndrome), chelation therapy may need to be introduced earlier because of the faster development of moderate-to-severe anemia before adequate iron removal is achieved.
For further reading, I would recommend the UpToDate card on treatment of hereditary hemochromatosis, authored by Drs. Stanley Schrier and Bruce Bacon, which highlights these discussion points.








interesting