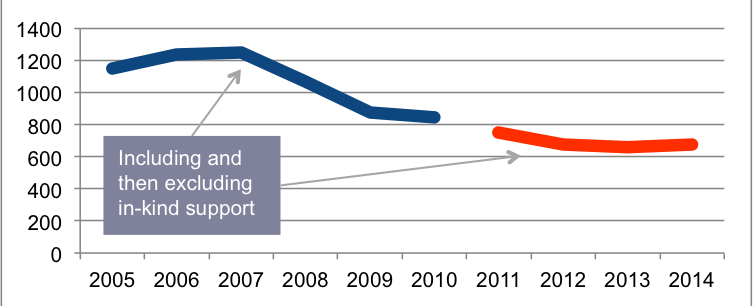
Regardless of where one stands in the debate around commercially funded CME for physicians, there is no question that industry support for CME has been falling over the past seven years. Statistics tracked by the Accreditation Council for Continuing Medical Education (ACCME), show a dramatic decline in commercially funded CME, though the rate of decline cannot be calculated precisely due to reporting changes made in 2011 by the ACCME to exclude in-kind commercial support.
Total Commercial Support for Accredited CME
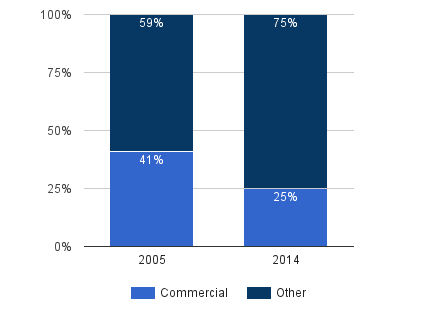
The total number of CME providers has also declined sharply over the same time period – by some 500+ providers or 26% in total – with medical education communication companies (MECCs) taking the biggest hit as CME grant monies have migrated to medical professional societies and schools of medicine. MECCs have long been a lightening rod for controversy around commercially funded CME as they have typically been formed for the sole purpose of expanding markets for prescription drugs.
One outcome of reduced industry funding for CME seems clear: physicians are paying more out of pocket to satisfy their CME requirements. According to statistics tracked by the ACCME, CME providers’ ‘income from other sources’, which includes participant registration fees, government grants, private donations, and allocations from a provider’s parent organizations or other internal departments, rising dramatically since 2007.
CME for Physicians: Income from Other Sources
While the physician community itself has been active in driving the decline in commercial funding for CME, this particular outcome may not be a welcome one. For example, an Archives of Internal Medicine study conducted in 2011 by Jeffrey Tabas, MD, and colleagues from the University of California at San Francisco found that, while nine in 10 physicians and other health care professionals believed industry funding raises the risk of biased CME, only 42% were actually willing to pay higher registration costs to eliminate commercial support altogether.
Of note is that ACCME’s latest Annual Report (2014) does show a leveling off in the trend for industry-backed CME; commercially funded CME actually ticked up 2.4% in 2014 when compared to 2013. Still, physician opposition or non-opposition to industry backed CME is only a small part of a much larger picture.
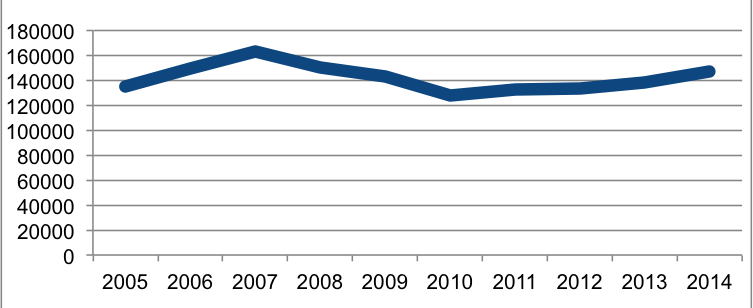
Total CME Activities Offered by Accredited Providers
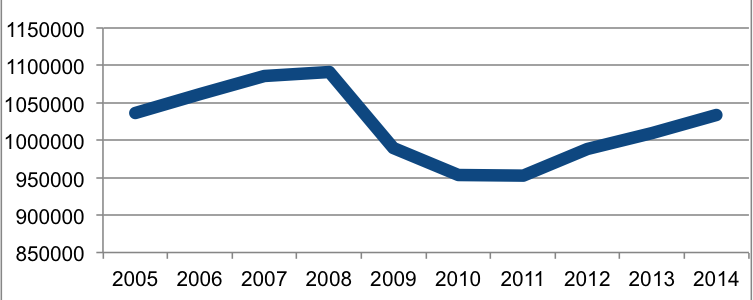
Total CME Hours Offered by Accredited Providers
Stepping back a few paces reveals four megatrends that would seem to suggest the slide in commercial funding for CME is here to stay.
Trend 1: Direct-to-Consumer Advertising
To fully understand the downtrend in commercially funded CME, it is perhaps necessary to go back nearly two decades to 1997 when the FDA first issued draft guidance relaxing constraints on direct-to-consumer (DTC) advertising by pharmaceutical companies. The FDA move, finalized in 1999, led to a boom in pharma print advertising directly to consumers. Additional FDA relaxation in 2004 – which made it permissible for pharma companies to present only information on major risks in language simplified for consumers – made the economics of broadcast and digital advertising much more attractive to pharma companies.
Annual DTC advertising skyrocketed from just $330 million in 1995 to over $5 billion by 2006-2007, when industry support for CME was reaching its peak. While DTC spending eroded to the $3-$4 billion range annually throughout the Great Recession, it has since been creeping back upward, consuming funds that, in the past, might have been earmarked for CME grants.
Trend 2: Physician Discretion Erodes
At the same time that pharmaceutical companies have been increasing direct influence over consumers through DTC advertising, insurance companies, hospitals, and government – motivated primarily by cutting health care costs — have been chipping away at physician discretion over which drug brands, medical devices, equipment, and even which clinical treatment pathways they can choose.
Multiple Supreme Court decisions solidifying Affordable Care Act (ACA or Obamacare) provisions over the past two years would seem to ensure that this erosion of physician discretion will continue as well. Even if pharmaceutical and medical device manufacturers could influence physician decisions via accredited CME — and this is a hotly debated question — industry’s motivation to even try has been declining for nearly two decades.
Trend 3: Public Opinion Turns, Inspiring Lawmakers to Regulate
By the mid-2000s – perhaps an outcome of massive growth in DTC advertising – the public began to demand that pharmaceutical companies stop attempting to influence physicians’ decisions. An article published by Public Citizen’s Commercial Alert in 2005 declared that the public’s perception of pharmaceutical companies had reached an all-time low:
Less than 13% of U.S. consumers believe information provided by pharmaceutical companies is more trustworthy than healthcare information provided by other organizations, according to new research. The research also found that public opinion has the potential to negatively impact individual pharmaceutical firms far more dramatically than increased federal regulations.
The report went on to state that:
Consumers who view information provided by pharmaceutical companies with suspicion may be less likely to approach a physician for treatment, preferring instead to remain untreated or rely on over-the-counter and herbal remedies. In addition, consumers who do seek medical help may be less likely to fill or refill a prescription.
The public inspired federal legislators and regulators to take a much keener interest in pharmaceutical company marketing practices — including in CME. This resulted in a series of both regulations and new laws targeting commercially funded CME directly. First, in the mid 2000s, both the FDA and Office of the Inspector General (OIG) issued guidelines seeking to influence how pharmaceutical manufacturers support CME. In 2006, Pharma Marketing News published a transcript of an industry roundtable discussion, providing key insights into industry perspectives on the subject of CME funding at the time. Roundtable participant John Kamp, Executive Director of the Coalition for Healthcare Communication, described the situation as follows:
Lately in the CME area we’ve been seeing “regulation by raised eyebrows,” by which I mean the chilling effect of such things as letters from Senator Grassley to pharmaceutical CEOs questioning a whole range of pharmaceutical marketing activities including CME. Virtually everything he’s been asking about is clearly illegal and not done by companies – at least not anymore – or covered by PhRMA guidelines for gifts to physicians. Some practices he’s questioning are clearly legal and he seems to be setting the stage for making them illegal or threatening to do so. I think this is a very serious threat because government regulation by raised eyebrows causes companies to avoid CME while this uncertainty prevails. The risk-of-censure game is just not worth the candle.”
That governmental pressure continued over subsequent years, culminating with the Physician Payments Sunshine Act, which Congress passed as part of the Affordable Care Act in 2010. Beginning in August of 2013, the Sunshine Act required manufacturers and Group Purchasing Organizations (GPOs) to report all payments and transfers of value to physicians and teaching hospitals to the Centers for Medicaid and Medicare Services (CMS), which would then aggregate and make the information available through a publicly searchable database.
In 2011, the CMS released initial reporting guidelines stating that all commercially supported CME would be reported as physician payments. Physicians either speaking at or attending commercially funded CME suddenly needed to start worrying about how this might affect their personal reputations and brands in the healthcare marketplace. Final rules published in February of 2013 backed off somewhat from the original CMS position, exempting commercially funded CME that had also been accredited by any of the following five organizations: ACCME, AMA, AAFP, AOA, or ADA CERP.
The clarification, however, created a different set of unforeseen reverberations in the CME realm. For example, because the Sunshine Act did not cover physician assistants (PAs) or nurse practitioners (NPs), such organizations as the AAPA and AANP were left off the list of excluded CME accreditors. This prompted a joint letter from AAPA and AANP CEOs to the CMS describing the effects:
We are both experiencing declines in grants as a result of the CMS FAQ that does not appropriately list us among the excluded accrediting organizations, and expect this to continue. The Sunshine Act is causing a shift in funding away from non-physician CME/CE towards physician CME due to the ‘safe harbor’ created only for physician CME organizations. The omission of AAPA and AANP as exempted accreditors means participation by physicians as speakers or attendees will be subject to a reporting system that will not exist for CME offered by organizations representing physicians.
In October, a new bill was introduced in the U.S. Senate that would add PAs and NPs to Sunshine Act reporting. While the bill might help to clarify matters in terms of reporting exemptions, the continuously shifting landscape and persistent scrutiny from lawmakers virtually assures that industry will remain cautious about backing CME while physicians and other healthcare workers will need to be careful about participating – either as faculty or attendees — in commercially backed CME events.
Trend 4: Wall Street Takes Aim at Pharma Cost Structures
A final factor suggesting the trend in commercially backed CME won’t recover anytime soon comes from within the pharma industry itself. Already by the mid-2000s, Wall Street analysts were calling for double-digit reductions in pharma-industry operating and capital costs. Economic and global market pressures on pharma have only continued to intensify since that time, and the industry faces several long-term structural challenges.
A forward-looking forecast from PriceWaterhouseCoopers, for example, predicts that a huge wave of patent expirations (the so-called ‘patent cliff’) and resulting competition from generic drugs will wipe roughly $148 billion from pharma industry revenues between 2012 and 2018. Other structural challenges cited in the PwC forecast include: flat-lining in the number of new medicines coming to market over the past decade, fast-rising costs to develop new drugs, and proliferation of government-led price controls throughout less mature global economies.
When FDA and OIG regulators forced pharma companies to divorce CME funding from brand marketing budgets in the mid-2000s, they also made CME budgets much more vulnerable to these industry long-term cost-cutting efforts. With the pie for CME shrinking overall, competition for industry grant monies should continue to intensify amongst professional societies, schools of medicine, publishers, MECCs, and other medical education providers.
More Fallout for CME for Physicians?
While it’s clear that physicians and other healthcare workers have been paying more out of pocket for mandated CME, proponents of commercially funded CME suggest the decline in industry backing since 2007 has also reduced both availability and accessibility of high-quality CME options. For example, a post appearing on the Policy and Medicine blog stated that:
What critics [of commercially funded CME] have failed to realize is that the decrease in financial resources, coupled with increased regulatory scrutiny and a difficult economy, have made providing high quality CME extremely difficult to produce. Consequently, a recent study confirmed these findings and showed that physicians believe there has been a decrease in the quality of CME programs.
The study referenced in that statement, however, was really an opinion poll of 515 doctors conducted by online physician portal MDLinx, which found some one in four physicians (26.6%) citing a decline in quality of CME programs, with the decline being tied only anecdotally to a “lack of authoritative speakers” and falloff in the “thoroughness of disease state education.” A strong majority (64.1%) of physicians participating in the MDLinx poll actually reported no change to CME quality while some 9.3% said CME quality was actually improving alongside the decline in commercial backing.
Other potential concerns raised in relation to declining industry support for CME include:
- Greater difficulty finding high-quality CME. For example, the same MDLinx poll found just over half of physicians (52.2%) stating they had increased time and effort spent locating appropriate CME.
- Less valuable debate and discourse as CME transitions more to individualized online and/or lower cost-to-produce options such as webinars.
- Rising risks of noncompliance with ACCME and other accreditation standards as grant monies migrate to organizations less experienced and adept than MECCS at navigating complex accreditation standards around financial interests and other disclosures.
- Potential for unintended consequences, such as an increase in non-accredited CME-style events competing with accredited CME for physicians’ already-stretched time and attention.
Aside from the one MDLinx opinion poll conducted back in 2011, however, there does not appear to be any substantive research or documentation either proving or disproving such fears as of yet. While the decline in commercially funded CME coincided initially with big drops in availability of accredited CME activities and hours of instruction, ACCME statistics show both areas rebounding strongly and steadily from 2010-2011 lows. Total hours of instruction, for example, which fell 13% from peak to trough between 2008 and 2011, had already regained some two-thirds of that loss (+8.5%) through 2014 as other CME providers, such as medical societies and schools of medicine have stepped in to fill gaps.
How Do You Feel About Commercially Funded CME for Physicians?
With these CME recovery trends in mind, we would be most interested in hearing commentary from our readers on the following questions:
- Have you personally noticed any changes in either the quality or accessibility of CME, since commercial funding began to decline in 2007?
- Have rising out-of-pocket costs influenced how you choose CME? For example, are you more likely to do just minimum requirements versus pursuing CME for sake of lifelong learning?
- Will you take advantage of more digital and online options for CME as a result of shifting trends?
- And are there areas where you see CME quality improving? Is technology helping in this respect?



In response:
Question 1: No
Question 2: Yes. The costs of the learning experience including travel, hotel and and registration fees, nature of the learning material/conference manifestly influences the choice of CME activity. As of now, I can meet my State’s minimum CME requirement (150hrs/3 years) for a total cost of $3.50/credit hour. This is the fee I pay to park in the lot of the local hospital where I attend weekly accredited CME lectures for free. I only attend those few specialty society CME sessions that have an annual attendance requirement.
Question 3: Definitely
Question 4: Definitely. Streaming Video and teleconferencing now allows for participation in the accredited CME activity from my home/office computer!
I was taught early on to use only the generic names of drugs in medical school (early 1980s), and although there were “drug lunches” in my first residency, these were not allowed by the late 80s during my second residency. I have never gone to an industry-sponsored CME event. I have participated in both on-site and by-mail then on-line CME and have noticed no decline in its quality, nor in the ease of obtaining it (and I always exceed my state’s CME requirement by at least 200 hours). I don’t trust the pharmaceutical industry to perform proper and unbiased studies and I never trust speakers with strong ties to one company. I trust most those with no ties to industry.
Thanks for the lovely information, we are also in the same field. Great Posting ……